Chronic Inflammation: Definition, Symptoms, Causes, Diet & How to Reduce It
Last updated: February 2026
Last reviewed for accuracy: February 2026
Quick answer:
Chronic inflammation is a long-term, low-grade immune response that can affect the body in different ways—often showing up as fatigue, aches, digestive discomfort, or ongoing “flare” patterns. The most reliable approach combines diet, sleep, movement, stress reduction, and targeted supplements—chosen based on your symptoms and triggers.
What you’ll learn in this guide:
- The inflammation definition/meaning and the 5 classic signs
- What causes inflammation in your body (and how to spot your triggers)
- The best inflammation diet + inflammation-reducing foods and foods to avoid
- How long can it take to reduce inflammation (realistic timeline)
- When to consider supplements and how to pick them (without overbuying)
Safety note:
Educational only. If you take medications (especially blood thinners) or have medical conditions, check with a qualified professional before changing diet, exercise, or supplements. Medical review: This page is not medically reviewed. It is written for educational purposes, using reputable clinical and public health references.
About the author
Daniel Popa is the founder of LiveGoodForLife, an independent wellness website focused on supplement education, ingredient analysis, and practical lifestyle strategies.
Daniel has studied naturopathy, herbalism, and natural medicine, and combines educational research with real-world product experience to help readers understand vitamins, minerals, performance supplements, and metabolic health support.
When reviewing supplements, Daniel focuses on ingredient transparency, label clarity, third-party testing disclosures (when available), pricing transparency, and safety considerations—so readers can make more informed decisions.
Important: Daniel is not providing medical care through this website. Content is educational and should not be used as a substitute for diagnosis or treatment from a qualified healthcare professional.
Editorial standards: Articles are written using reputable clinical and public-health references (e.g., NHS, NIH/NCBI, MedlinePlus, Mayo Clinic, Cleveland Clinic, WHO). Claims are written conservatively, and supplement guidance is framed around safety, symptom tracking, and when to seek medical care.
Affiliate disclosure: Some links may be affiliate links. If you purchase through them, LiveGoodForLife may earn a commission at no extra cost to you. This does not change the way products are evaluated.
Updates & corrections: Pages are reviewed periodically and updated when guidance changes or when we find an error. If you spot an issue, please contact us via the Contact page.
👉 Explore more of Daniel’s story and mission on the About page.

Related guide:
If you’re considering supplements, don’t guess or buy a dozen bottles at once—use our anti-inflammatory supplements guide to match options to your symptoms and goals.
Inflammation definition and meaning (what is inflammation?)
Inflammation is your body’s built-in defense and repair response. When your immune system detects injury, irritation, or infection, it sends signals and immune cells to protect the area, remove the threat, and start healing.
In simple terms, inflammation is what happens when your body “turns on” protection mode—sometimes briefly (helpful), sometimes for too long (not helpful).
The 5 classic signs of inflammation (quick bullets)
- Redness
- Heat
- Swelling
- Pain
- Loss of function (the area doesn’t work normally)
Acute vs chronic inflammation (simple comparison)
Acute inflammation is short-term and usually tied to a clear cause (like a cut or infection). Chronic inflammation is long-term, lower-grade, and can be driven by repeated triggers (diet, sleep debt, stress load, inactivity, metabolic strain, ongoing irritants).
Acute vs chronic inflammation (duration, common triggers, common patterns)
| Type | Duration | Common triggers | Common patterns |
|---|---|---|---|
| Acute inflammation | Hours to days (sometimes weeks) | Injury, infection, short-term irritation | Sudden pain, swelling, warmth; improves as the issue resolves |
| Chronic inflammation | Months to years | Ongoing lifestyle stressors, persistent irritants, immune-related conditions, metabolic strain | “Always there” fatigue/aches, recurring flare cycles, lingering discomfort |
What does inflammation feel like?
Inflammation can feel obvious (like a swollen ankle) or subtle (like persistent fatigue that never fully lifts). Many people describe it as a background “noise” in the body—aches, puffiness, heaviness, or flare patterns that come and go.
How do you tell if your body is inflamed?
You’re looking for patterns, not one random bad day. A practical way to tell is to watch for symptoms that:
- show up most weeks, not just occasionally
- worsen after common triggers (poor sleep, alcohol, ultra-processed meals, high stress)
- improve when you get consistent with sleep, movement, and whole foods
If symptoms are severe, progressive, or accompanied by alarming signs (unexplained weight loss, fever, chest pain, blood in stool), seek medical guidance promptly.

What are the 10 signs of chronic inflammation?
These are common “red flags” people notice when inflammation is more persistent (not a diagnosis—just a signal to investigate):
- Ongoing fatigue or low energy
- Frequent aches or joint stiffness
- Morning stiffness that takes time to loosen
- Digestive discomfort (bloating, irregularity, sensitivity)
- Brain fog or poor focus
- Sleep issues (trouble falling asleep, waking unrefreshed)
- Frequent headaches or “pressure” feelings
- Skin flare patterns (varies by person)
- Slow recovery after workouts or normal activity
- Mood changes linked to stress/sleep dips (irritability, low mood)
What are the three warning signs of inflammation?
If you want the simplest “watch list,” focus on these three:
- Persistent fatigue (energy doesn’t rebound with rest)
- Ongoing aches/stiffness (especially morning stiffness)
- Recurring digestive issues (bloating, discomfort, irregularity)
When these cluster together, it often points to lifestyle triggers worth addressing—starting with sleep, food quality, stress load, and movement.
Symptom tracker you can screenshot (energy, stiffness, digestion, sleep)
- Energy (1–10): ____
- Stiffness/aches (0–10): ____
- Digestion (0–10): ____ (bloating, discomfort, regularity)
- Sleep quality (1–5): ____ (time in bed + how you felt on waking)
- Notes (possible triggers today): alcohol / ultra-processed foods / high stress / low movement / poor sleep
What causes inflammation in your body?
Inflammation is triggered when your immune system detects a threat (like infection or injury). But inflammation can also stay “switched on” when triggers repeat over time—especially from lifestyle stressors like poor sleep, highly processed diets, chronic stress, inactivity, smoking, or metabolic strain. For a medical overview of how inflammation works (and why chronic inflammation matters), see What Is Inflammation? Types, Causes & Treatment.
Common lifestyle triggers (food, sleep, stress, inactivity)
Here are the most common modifiable drivers people run into:
- Food pattern triggers: frequent ultra-processed foods, high added sugar, and low fiber. If you want a practical “what to eat” framework, see Harvard’s evidence-based overview of an anti-inflammatory pattern: Diet Review: Anti-Inflammatory Diet.
- Sleep debt: poor sleep and sleep disruption are associated with changes in inflammatory markers in research reviews. If you want the science summary, see Sleep Disturbance, Sleep Duration, and Inflammation.
- Chronic stress load: long-term stress can affect immune function and amplify inflammatory signaling. For a clear explanation, see What Happens When Your Immune System Gets Stressed Out?.
- Low movement / sitting most of the day: regular activity supports overall health and helps counter the downsides of a sedentary routine. For baseline guidelines and why it matters, see the WHO fact sheet: Physical activity.
How do I figure out what is causing inflammation in my body?
Use a simple “one change at a time” approach so you don’t get lost:
- Pick one anchor symptom (fatigue, morning stiffness, bloating, headaches, flare cycles).
- Track 4 basics daily for 14 days: sleep, food quality, alcohol, movement.
- Test one trigger at a time for 14 days (not all at once).
- Re-check your symptom tracker and keep what works.
Trigger → what to test for 14 days (sleep, alcohol, sugar, ultra-processed foods, low movement)
| Trigger | What to test for 14 days | What “improvement” looks like |
|---|---|---|
| Sleep debt | Same bedtime/wake time + aim for 7–9 hours in bed | Better morning energy, fewer cravings, steadier mood |
| Alcohol | Remove alcohol completely | Better sleep quality, less puffiness, improved digestion |
| Added sugar | Cut sweet drinks + dessert most days | Fewer energy crashes, less afternoon fatigue |
| Ultra-processed foods | Replace 1–2 meals/day with whole-food meals | Less bloating, fewer “flare” patterns |
| Low movement | 20–30 min walk daily (or 8–10k steps) | Less stiffness, better sleep, better digestion |
How to reduce inflammation in the body (natural plan)
For many people, the most reliable starting point is consistent food quality + sleep + movement + stress recovery, then supplements only if they match your symptom pattern, goals, and safety profile. For a clinical overview of chronic inflammation (including why it can linger), see Chronic Inflammation (StatPearls).
How to get rid of inflammation in the body (step-by-step)
Step 1: Build an anti-inflammatory plate (most meals)
- Half plate: vegetables + fruit
- Quarter plate: protein
- Quarter plate: high-fiber carbs (beans, oats, whole grains)
- Add healthy fats (olive oil, nuts, seeds)
For research context on why Mediterranean-style eating is often recommended, see this systematic review/meta-analysis: Mediterranean Diet Reduces Inflammation in Adults.
Step 2: Fix sleep first (highest ROI for many people)
Prioritize consistent sleep timing and enough total sleep. For the research summary, see Sleep Disturbance, Sleep Duration, and Inflammation.
Step 3: Move daily (consistency beats intensity)
- Walk daily (especially after meals)
- Add light strength training 2x/week if appropriate
Step 4: Reduce stress input + increase recovery output
You don’t need perfect meditation—start with 10 minutes/day of something downshifting (walk outside, breathwork, journaling, prayer, stretching). For a practical overview of stress and immune effects, see What Happens When Your Immune System Gets Stressed Out?.
Step 5: Add targeted supplements only if needed
Start with one supplement, track your anchor symptom for 3–8 weeks, and only then decide whether to continue or add something else.
How long does it take to reduce inflammation in the body?
A realistic timeline (varies by cause and consistency):
- 3–7 days: sleep and digestion may improve if you remove alcohol/sugary drinks and stop late-night eating
- 2–4 weeks: energy and stiffness patterns often improve with daily walking + fiber + consistent sleep
- 8–12+ weeks: deeper changes (weight, metabolic markers, longer-term flare patterns) typically take longer
Note: Timelines vary widely depending on the underlying cause, baseline health, and consistency—use this as a general expectation, not a guarantee.
Can chronic inflammation ever go away?
Often, it can improve significantly when the main drivers are addressed—especially when inflammation is linked to lifestyle triggers. Some causes are medical (autoimmune disease, persistent infections, inflammatory bowel disease, etc.) and require diagnosis + treatment. For a clinical overview, see Chronic Inflammation (StatPearls).
Self-care vs get checked (red flags)
Try self-care first (2–4 weeks) if symptoms are mild/moderate, and you’re otherwise well:
- fatigue, aches, mild digestive discomfort, mild stiffness
- clear links to sleep/diet/stress
- no “alarm” symptoms
Get checked promptly if you have any of these red flags:
- chest pain, trouble breathing, fainting
- fever that persists, unexplained weight loss
- blood in stool, black/tarry stool, severe abdominal pain
- sudden swelling/pain in one limb, severe new headaches
- symptoms steadily worsening despite basic changes
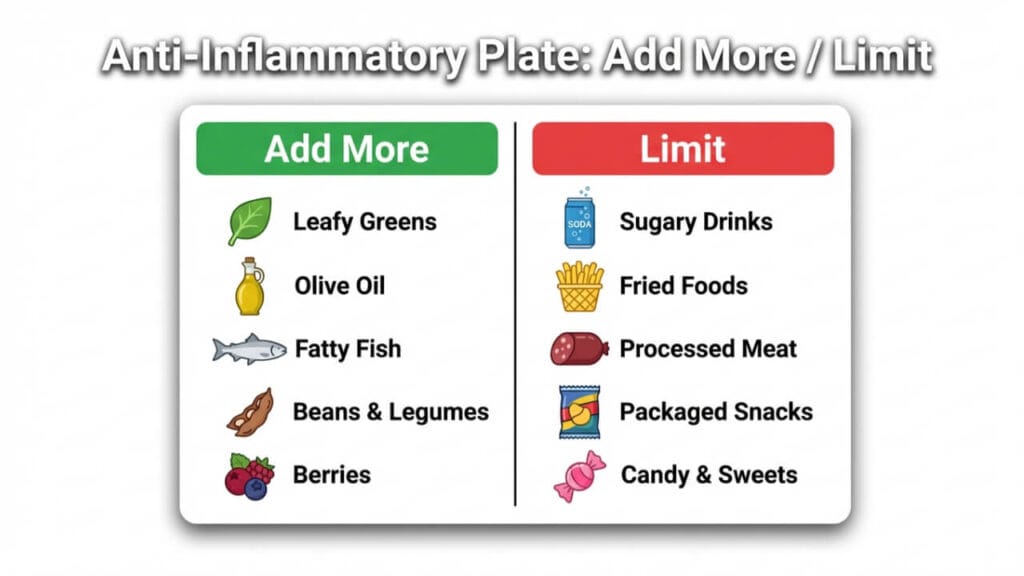

Inflammation diet (what to eat + what to avoid)
The best-supported “inflammation reduction diet” looks a lot like a Mediterranean-style pattern: more plants, more fiber, healthy fats (especially olive oil), and fewer ultra-processed foods. For a clear, practical breakdown, see What is the Mediterranean Diet? from the American Heart Association.
Inflammation-reducing foods (what to eat daily)
Aim to include several of these most days:
- Colorful vegetables and fruit (especially berries)
- Beans, lentils, chickpeas (high fiber)
- Nuts and seeds
- Extra-virgin olive oil
- Fatty fish (omega-3s)
- Herbs/spices (like turmeric, ginger)
For a simple food list you can skim quickly, see Foods that fight inflammation.
Inflammatory foods to avoid (high-impact swaps)
If you only change a few things, make it these:
- Sugary drinks → swap to water/sparkling water/unsweetened tea
- Ultra-processed snacks → swap to fruit + yogurt, nuts, or hummus + veg
- Refined carbs as default → swap to oats, whole grains, beans/lentils
- Processed meats (bacon/sausages/deli meats) → swap to fish, poultry, beans
If you want a “start gradually” substitution strategy (with examples), see Anti-inflammatory diet from Johns Hopkins Medicine.
If you’re searching for “10 worst inflammatory foods”, these are common high-impact categories to reduce:
- sugary drinks
- candy/desserts most days
- deep-fried foods
- processed meats
- packaged snacks high in refined carbs + oils
- fast food meals as a frequent default
What foods clear up inflammation?
No single food “clears” inflammation overnight—but a consistent pattern that increases fiber, plants, omega-3s, and reduces ultra-processed foods can shift inflammatory balance over time. For research context, see Mediterranean Diet Reduces Inflammation in Adults.
| Add more of | Limit |
|---|---|
| Vegetables (especially leafy greens) | Sugary drinks |
| Berries and whole fruit | Processed meats |
| Beans/lentils/oats (fiber) | Ultra-processed snacks |
| Extra-virgin olive oil | Frequent fried foods |
| Fatty fish (omega-3s) | Refined carbs as the default |
| Nuts/seeds | Alcohol “stacking” (many days in a row) |
Inflammatory foods (quick answers people search)
What are “inflammation foods”? People usually mean foods and drinks that can increase inflammation over time (especially ultra-processed, high-sugar patterns) versus foods that tend to support a healthier inflammatory balance (fiber-rich plants, healthy fats, omega-3 sources).
What drink kills inflammation? (hydration + beverage habits)
No drink “kills” inflammation instantly. The most reliable beverage habit is simple: drink enough water consistently and avoid turning drinks into sugar delivery systems.
If you want evidence-backed beverage options that may support an anti-inflammatory pattern, coffee and tea are commonly discussed because they contain polyphenols (antioxidant compounds). For a balanced overview, see Which is healthier: Coffee or tea?.
- Best default: water or sparkling water
- Also helpful: unsweetened tea, black coffee (if tolerated)
- Watch-outs: sugary coffees/teas, juices used like “sports drinks,” energy drinks
The 5 worst foods for inflammation
To keep this practical and neutral, these are the most common high-impact categories people benefit from reducing (especially when they’re daily staples):
- Sugary drinks (soda, sweetened coffees, sweet teas)
- Ultra-processed snack foods (chips, packaged sweets, “grab-and-go” pastries)
- Processed meats (bacon, sausages, deli meats)
- Deep-fried fast foods (frequent fried meals as a default)
- Refined carbs as the default (white bread/pasta/pastries replacing fiber-rich staples)
If you want a food-first, evidence-based anti-inflammatory framework (without extremes), Harvard’s overview is a solid starting point: Foods that fight inflammation.
Inflammation in the intestines and colon (gut inflammation basics)
“Inflammation in the intestines” or “colon inflammation” can describe many different situations—from short-term irritation to medical conditions that need evaluation. This section is non-diagnostic and focused on common patterns and when to seek care.
Common patterns (bloating, discomfort, irregularity) — non-diagnostic
People often search these terms when they notice:
- Bloating or a “tight” abdomen after meals
- Discomfort (cramps, pressure, or sensitivity)
- Irregularity (constipation, diarrhea, or alternating patterns)
- Food-related flare patterns (certain meals consistently worsen symptoms)
Diet basics that often help gut inflammation (fiber, trigger reduction)
For many people, the “big wins” are less about one perfect food and more about building a calmer baseline:
- Go slower with fiber increases: if you’re currently low-fiber, increase gradually to reduce gas/bloating.
- Reduce ultra-processed foods and added sugar for 14 days and watch your symptom tracker.
- Identify your “repeat offenders” (common ones include large fatty meals, alcohol, very spicy foods, and sugar alcohols in “diet” snacks).
- Use a simple meal structure: protein + cooked veg + easy carb (rice/oats/potatoes) when your gut feels sensitive.
If you’re experiencing ongoing bowel changes with blood, that’s a “do not ignore” category. NIDDK’s overview explains how blood in stool or black/tarry stool can signal GI bleeding and should be evaluated: Symptoms & Causes of GI Bleeding.
When to get checked (GI red flags)
Get medical advice promptly if you have:
- Blood in stool or black/tarry stool
- Persistent diarrhea, severe constipation, or dehydration
- Severe abdominal pain, fever, or symptoms that rapidly worsen
- Unexplained weight loss or persistent vomiting
For clear “urgent symptoms” guidance related to bowel inflammation conditions, the NHS guidance on inflammatory bowel disease includes emergency warning signs (like severe pain or heavy bleeding): Inflammatory bowel disease (NHS).
Inflammation in the stomach (gastritis) — what it may mean
“Inflammation in the stomach” is commonly referred to as gastritis—inflammation or irritation of the stomach lining. It can be short-term (acute) or long-lasting (chronic), and symptoms vary from person to person.
For a straightforward medical definition and symptom overview, see MedlinePlus: Gastritis (MedlinePlus).
Common triggers (food, stress, meds) — neutral
Common triggers and contributors can include:
- NSAID use (like ibuprofen/aspirin) for some people
- Alcohol or frequent irritation from very spicy/acidic foods (individual tolerance varies)
- High stress load (often worsens symptoms and coping behaviors)
- Infection (H. pylori) is a common medical cause (requires testing/treatment)
Mayo Clinic summarizes common causes and also notes when to seek medical care for gastritis symptoms: Gastritis: Symptoms and causes.
Gentle food approach (temporary + practical)
If your stomach feels irritated, a short-term “gentle” approach can help you stabilize while you track triggers (this isn’t a forever diet):
- Smaller, simpler meals (avoid huge late-night portions)
- Lean protein + easy carbs (rice, oats, potatoes) + cooked vegetables
- Pause alcohol and reduce very spicy, very acidic, and very fatty meals for 7–14 days
- Limit irritating add-ons (carbonated sugary drinks, heavy caffeine if it worsens symptoms)
Also consider the context: if symptoms began after starting (or increasing) NSAIDs, that’s a useful clue to bring to a clinician.
When should symptoms be evaluated
Seek medical care sooner if symptoms are persistent (a week or longer), severe, or worsening. Get urgent care if you have severe pain, can’t keep food down, feel faint/dizzy, or notice vomiting blood or black stools. Mayo Clinic lists these warning signs here: When to seek medical attention for gastritis.
Inflammation for Arthritis and Knee Joint Discomfort
When people search “inflammation for arthritis” or “inflammation knee joint,” they’re usually looking for practical ways to reduce pain, stiffness, and limited mobility. While supplements get a lot of attention, most clinical guidance starts with movement, strength, and recovery habits because they’re high-impact and low-cost.
For a clear medical overview of osteoarthritis treatment steps (including exercise to reduce pain and stiffness), see Osteoarthritis: Diagnosis, Treatment, and Steps to Take (NIAMS).
Mobility + stiffness routines (movement + recovery)
Think “gentle daily motion + 2–3x/week strength + recovery.” The goal is to keep the joint moving, support it with stronger muscles, and reduce flare-ups caused by doing too much on one day and nothing for a week.
- Daily mobility (5–10 minutes): easy range-of-motion + short walk.
- Strength (2–3x/week): focus on quads, glutes, hamstrings, calves (knee support muscles).
- Low-impact cardio: cycling, swimming, elliptical, or walking if tolerated.
- Heat before / cold after (optional): some people find heat helps loosen stiffness pre-movement and cold helps post-activity soreness.
If you want a practical, mainstream guide on exercise for arthritis pain and stiffness (including low-impact ideas), see Exercise helps ease arthritis pain and stiffness (Mayo Clinic).
Supplements people commonly research for joints (tease your supplements post)
People commonly research these for joint discomfort: omega-3s, curcumin/turmeric, glucosamine/chondroitin, collagen peptides, and boswellia. Results vary by person, dose, and product quality—so it’s best to treat supplements as “support,” not the main plan.
For balanced evidence summaries (including safety and medication interactions), see:
Teaser: I break down “which supplement fits which joint pattern,” how to choose quality, and what to avoid in the dedicated supplements post (so you don’t overbuy).
Inflammation of the liver (and “inflammation to liver”)
When someone searches “inflammation liver” or “inflammation to liver,” they’re often reacting to a lab result (like elevated liver enzymes) or symptoms like fatigue, right-upper abdominal discomfort, or concern about alcohol/medications.
What this search usually means (general education; not diagnosing)
Many people are really asking: “Do my results suggest liver irritation or injury?” Medical sources explain that elevated liver enzymes can be a sign of inflamed or damaged liver cells, but the cause can range from temporary to more serious—and it requires context.
For a concise definition of what elevated liver enzymes can indicate (and which enzymes are commonly discussed), see Elevated liver enzymes (Mayo Clinic).
For a broad overview of liver disease categories and common causes of liver inflammation (including viral hepatitis and alcohol/drug-related causes), see Liver Disease (NIDDK).
When lab work matters (talk to clinician)
If you’re worried about “liver inflammation,” lab work is often where clinicians start—especially if symptoms persist or you have risk factors. A key point: liver panels can show that something is off, but they usually can’t identify the exact cause on their own without follow-up and medical context.
For a patient-friendly explanation of what liver function tests are and what they can (and can’t) tell you, see Liver Function Tests (MedlinePlus).
Important: If you have yellowing of the skin/eyes, severe abdominal pain, confusion, vomiting blood, or black/tarry stools, seek urgent care.
Inflammation lab test (what people ask doctors for)
When people ask for an “inflammation lab test,” they usually mean a blood test that can detect inflammation in the body. These tests can be useful, but they’re not location-specific—they don’t automatically tell you why inflammation is happening or exactly where it’s coming from.
Common markers people discuss (general)
Two of the most commonly discussed inflammation markers are:
- CRP (C-reactive protein): a general marker that can rise with inflammation from many causes. Learn more here: C-Reactive Protein (CRP) Test (MedlinePlus).
- ESR (erythrocyte sedimentation rate): another general inflammation marker used in many clinical situations. Learn more here: Erythrocyte Sedimentation Rate (ESR) (MedlinePlus).
Depending on symptoms, clinicians may also consider other labs (CBC, metabolic panels, thyroid tests, autoimmune markers, stool tests, etc.). The best test is the one matched to your symptoms and exam—not the most popular one online.
How to use tracking + clinician guidance together
A smart approach is to combine your symptom tracker with medical guidance:
- Track first: energy, stiffness, digestion, sleep, alcohol, and ultra-processed meals for 14 days.
- Bring patterns to the appointment: “My joint stiffness is worse after poor sleep,” or “my gut flares after alcohol + fried foods.”
- Ask targeted questions: “Would CRP/ESR help here?” “Do we need liver tests?” “Are there red flags that require imaging or specialist referral?”
- Use labs as feedback: track symptoms over time and re-check only if clinically appropriate.
Safety note: If you’re taking medications (especially blood thinners) or you have diagnosed conditions, ask your clinician before starting new supplements—even “natural” ones can interact.
Inflammation medication and drugs (educational overview)
When people search “inflammation medication” or “inflammation drugs,” they’re usually trying to figure out what doctors use to reduce pain, swelling, or immune-driven inflammation. This section is educational and non-prescriptive—the right option depends on your symptoms, medical history, and risk factors.
As a starting point, MedlinePlus summarizes common medication categories used for inflammatory conditions like arthritis (including anti-inflammatory pain relievers and prescription options): Medicines, injections, and supplements for arthritis (MedlinePlus).
Important: Don’t start, stop, or combine anti-inflammatory medicines without a clinician’s advice—especially if you have a history of ulcers/bleeding, kidney disease, heart disease, liver disease, asthma, or you take blood thinners.
What medication is used for chronic inflammation?
“Chronic inflammation” can come from many causes, so clinicians choose medication based on what’s driving it:
- Symptom relief (pain/inflammation): Non-steroidal anti-inflammatory drugs (NSAIDs) are commonly used to reduce pain and inflammation in many conditions.
- Short-term flare control: corticosteroids may be used in some inflammatory conditions to reduce inflammation more quickly, but they carry important risks and are usually managed carefully by a clinician.
- Immune-driven inflammation (autoimmune arthritis, etc.): disease-modifying antirheumatic drugs (DMARDs) are used to treat certain autoimmune conditions by targeting the disease process, not just symptoms.
If you want an overview of NSAIDs (what they are, what they’re used for, and key cautions), see NSAIDs (NHS).
If your inflammation is linked to autoimmune arthritis, Cleveland Clinic explains what DMARDs are and why they’re used to manage immune-driven inflammation: Disease-Modifying Antirheumatic Drugs (DMARDs) (Cleveland Clinic).
What is the best medicine for chronic inflammation? (general, non-prescriptive)
There isn’t one “best” medicine for chronic inflammation because the cause matters. For example:
- If the driver is mechanical wear-and-tear (like osteoarthritis), treatment often focuses on movement/strength, weight management (if applicable), and symptom relief strategies.
- If the driver is autoimmune inflammation (like rheumatoid arthritis), clinicians often use DMARDs to slow the disease process, with other meds layered in as needed.
- If the driver is infected or has another medical condition, treating the underlying issue is the priority—not simply suppressing inflammation.
A practical takeaway: the “best medicine” is the one matched to (1) your diagnosis, (2) your risk profile, and (3) your symptom severity—after a clinician reviews your history and any relevant labs/imaging.
What is the strongest anti-inflammatory drug? (explain why “strongest” depends)
“Strongest” depends on what you mean by strong:
- Fast symptom reduction: some medications can reduce inflammation quickly, but may have higher short- and long-term risks.
- Long-term disease control: other medications are considered “strong” because they can slow immune-driven disease activity over time—not because they give instant relief.
- Safety trade-offs: a medicine may be “stronger” for inflammation but not appropriate for someone with certain medical risks (ulcers, kidney disease, heart disease, blood thinners, etc.).
For a clinician-reviewed explanation of NSAIDs—including common side effects and why you shouldn’t take them long-term without guidance—see Cleveland Clinic’s overview: NSAIDs (Nonsteroidal Anti-Inflammatory Drugs): Uses (Cleveland Clinic).
Note: If you’re asking medication questions, it’s worth a short clinician conversation. Bring your symptom tracker, list your current medications/supplements, and ask: “What’s the safest option for my situation, and what should I watch for?”

Supplements that may help with inflammation (how to choose)
If you’re searching for “inflammation pills,” the biggest mistake is buying 5–10 supplements at once and then having no idea what helped. A smarter approach is: pick a goal → choose one supplement → track results for 3–8 weeks before adding anything else. Start Here: How We Evaluate LiveGood Supplements
Quick safety note: If you take medications (especially blood thinners), have medical conditions, or you’re pregnant/breastfeeding, talk to a qualified clinician before starting supplements. Even “natural” options can interact with medications.
- Step 1: Choose your main goal (joints, gut, stress-sleep, recovery).
- Step 2: Choose one supplement that matches that goal.
- Step 3: Track one anchor symptom (e.g., morning stiffness, bloating, sleep quality) for 3–8 weeks.
- Step 4: Keep / stop based on results (don’t keep paying for “maybe”).
Which 3 supplements fight chronic inflammation?
There’s no perfect “top 3” for everyone, but these are three of the most commonly researched categories because they match common inflammation patterns (joints, gut, overall):
- Omega-3s (EPA/DHA) – commonly researched for joint comfort, recovery, and overall inflammation support (dose and product quality matter).
- Curcumin (turmeric extract) – commonly researched for general inflammation support; absorption/formulation matters.
- Probiotics – commonly researched when symptoms look gut-driven (bloating, irregularity, “flare” patterns); results vary by strain and consistency.
For the full breakdown (including how to pick a quality product, who should avoid certain supplements, and the “best choice by symptom”), use our dedicated guide: The Ultimate Anti-Inflammatory Guide.
Inflammation turmeric (why it’s searched so much)
“Inflammation turmeric” because turmeric contains curcumin, a compound studied for its role in inflammation pathways. The key detail most people miss: turmeric powders and capsules vary widely, and many curcumin supplements are designed for better absorption than plain turmeric.
For an evidence-based and safety overview (including side effects and medication interactions), see Turmeric: Usefulness and Safety (NCCIH).
Practical takeaway: If you’re trying turmeric for inflammation, track one outcome (like morning stiffness or post-workout soreness) for a few weeks, and stop if you don’t see a meaningful difference.
Supplements by goal: joints/gut / stress-sleep
| Goal | Supplements people commonly research | What to track (simple) |
|---|---|---|
| Joints | Omega-3s (EPA/DHA), curcumin/turmeric, boswellia, collagen peptides | Morning stiffness (minutes), pain after activity (0–10) |
| Gut | Probiotics (strain-dependent), fiber (gradual increase), peppermint oil (some cases) | Bloating (0–10), regularity, trigger meals |
| Stress + sleep | Magnesium (sleep support for some), L-theanine (calm focus for some) | Sleep quality (1–5), next-day energy (1–10) |
Keeping supplement costs low (member vs retail pricing)
The simplest way to get results with an inflammation-focused routine is to keep it affordable enough to stay consistent. If the monthly cost feels realistic, you’re far more likely to stick with your plan long enough to notice real changes—then adjust based on what your body responds to.
That’s why member vs retail pricing matters: it turns supplements from a “short trial” into something you can actually keep doing week after week. How to Reduce Inflammation Naturally and Feel Your Best– The Ultimate Anti-Inflammatory Guide.
Why consistency matters more than chasing “perfect.”
When the goal is lowering inflammation, a repeatable routine usually wins. A steady plan built on diet basics + sleep + movement, plus one targeted supplement, often beats an expensive stack you stop after two weeks.
- Pick one goal: joints, gut, or overall inflammation support.
- Choose one product you can comfortably take every day.
- Track one anchor symptom (morning stiffness, bloating, sleep quality) for 3–8 weeks.
- Keep what works and drop what doesn’t.
LiveGood product options aligned with inflammation topics
Here are a few LiveGood options that line up with the most common inflammation-related goals people search for. Click any product to see the full details.
Factor4 – Advanced Inflammation Management (all-in-one inflammation support)
If you want one product that targets inflammation from multiple angles, Factor4 is built as an all-in-one option—so you can test a single supplement consistently instead of stacking multiple bottles. It’s formulated with Fish Oil, Turmeric, Coenzyme Q10, and Garlic.
Member Price: 19.95 • Retail Price: 29.95
More Factor4 reads: Factor4: Fighting Inflammation | Reducing Inflammation With Factor4
Probiotic Gut Support (gut comfort & digestion support)
If your “inflammation” feels gut-driven (bloating, discomfort, irregularity), this is a straightforward place to start. It’s designed as a multi-support formula combining probiotics with digestive support—so you can test one product instead of buying several.
Member Price: 17.95 • Retail Price: 34.95
Osteo Complete – Advanced Bone Support (joint & mobility support context)
If your main concern is mobility and stiffness, this option is geared toward structural support. It’s a “broader formula” approach—useful for people who want one product that covers multiple support angles rather than stacking several separate bottles.
Member Price: 16.95 • Retail Price: 39.95
Premium Black Seed Oil – 5% Thymoquinone (overall inflammation-support interest)
This is a popular match for readers searching broadly for “inflammation support.” If you’re trying to keep things simple, it can fit as a single add-on while you focus on the bigger drivers (sleep, food quality, movement, stress recovery).
Member Price: 14.95 • Retail Price: 34.95
Quick reminder: Start with one product, run it for a few weeks, and track one measurable outcome. That’s how you avoid overbuying—and how you figure out what actually helps you.
Disclosure: Some links may be affiliate links. If you purchase through them, we may earn a commission at no extra cost to you.
Sources used (clinical & public health references)
To keep this guide accurate and safety-focused, I referenced the following clinician-reviewed and public-health sources:
- Cleveland Clinic – Inflammation overview: What Is Inflammation? Types, Causes & Treatment
- Harvard T.H. Chan School of Public Health – Anti-inflammatory eating pattern: Diet Review: Anti-Inflammatory Diet
- WHO – Physical activity guidelines (baseline): Physical activity
- NCBI Bookshelf (StatPearls) – Clinical overview of chronic inflammation: Chronic Inflammation
- PubMed – Mediterranean diet & inflammation (systematic review/meta-analysis): Mediterranean Diet Reduces Inflammation in Adults
- PMC (NIH) – Sleep and inflammation research review: Sleep Disturbance, Sleep Duration, and Inflammation
- American Heart Association – Mediterranean diet overview: What is the Mediterranean Diet?
- Harvard Health – Foods that support a healthier inflammatory balance: Foods that fight inflammation
- Johns Hopkins Medicine – Practical anti-inflammatory diet framework: Anti-inflammatory diet
- NIDDK (NIH) – GI bleeding symptoms & causes (red flags): Symptoms & Causes of GI Bleeding
- NHS – Inflammatory bowel disease overview & warning signs: Inflammatory bowel disease (IBD)
- MedlinePlus – Gastritis definition: Gastritis
- Mayo Clinic – Gastritis symptoms/causes and when to seek care: Gastritis: Symptoms and causes
- MedlinePlus – Inflammation markers: CRP Test and ESR Test
- NIAMS (NIH) – Osteoarthritis treatment steps: Osteoarthritis: Diagnosis, Treatment, and Steps to Take
- NCCIH (NIH) – Supplement evidence & safety: Turmeric and Glucosamine & Chondroitin
- NHS – NSAIDs overview & cautions: NSAIDs
Note: These sources provide general education. If you have persistent, severe, or worsening symptoms—or red flags like bleeding, chest pain, fainting, or unexplained weight loss—seek medical care promptly.
FAQ
How do you flush inflammation out of your body?
You can’t “flush” inflammation out overnight, but you can lower inflammatory load by stacking the basics: improve sleep, move daily, reduce ultra-processed foods and sugary drinks, and focus on fiber-rich whole foods. If symptoms persist or you have red flags (fever, chest pain, blood in stool, unexplained weight loss), get medical guidance.
What are the 5 classic signs of inflammation?
The 5 classic signs of inflammation are redness, heat, swelling, pain, and loss of function (the area doesn’t work normally).
What foods clear up inflammation?
No single food “clears” inflammation instantly. The most reliable approach is a consistent anti-inflammatory eating pattern: more vegetables and fruit, beans/lentils, nuts and seeds, olive oil, and omega-3 sources (like fatty fish), while reducing ultra-processed foods, added sugar, and frequent fried foods.
How do I reduce inflammation in my body?
Start with the highest-impact levers: sleep consistency, daily movement, whole-food meals, and stress recovery. Then add one targeted supplement only if it fits your goal (joints, gut, sleep/stress) and you can track whether it helps over 3–8 weeks.
How long does it take to reduce inflammation in the body?
It depends on the cause and how consistent you are. Many people notice early improvements (energy, digestion, sleep) within 1–2 weeks of cleaning up sleep and reducing alcohol/sugary drinks. Bigger changes often take 8–12+ weeks with a steady diet, movement, and recovery habits.
What are the 10 signs of chronic inflammation?
Common signs people notice include: ongoing fatigue, frequent aches or joint stiffness, morning stiffness, digestive discomfort (bloating/irregularity), brain fog, sleep issues, frequent headaches, recurring skin flare patterns, slow recovery, and mood changes linked to stress or poor sleep. If symptoms are severe or worsening, get checked.
Medical disclaimer
Important: This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. Inflammation can be caused by many different conditions, and the right approach depends on your personal health history and symptoms.
Always consult a qualified healthcare professional before making changes to your diet, exercise, medications, or supplements—especially if you:
- take prescription medications (particularly blood thinners, blood pressure meds, diabetes meds, or immune-modulating drugs)
- have a diagnosed medical condition (autoimmune disease, heart disease, kidney disease, liver disease, GI disorders, etc.)
- are pregnant, trying to conceive, or breastfeeding
- have a history of ulcers, bleeding, or medication sensitivities
Seek urgent care if you have warning signs such as chest pain, trouble breathing, fainting, severe abdominal pain, vomiting blood, black/tarry stools, a new, severe headache, persistent fever, or unexplained weight loss.
